In patients with type 2 diabetes mellitus, insulin may be used to augment therapy with oral glycemic medications or as insulin replacement therapy. The American Diabetes Association suggests the use of long-acting (basal) insulin to augment therapy with one or two oral agents or one oral agent plus a glucagon-like peptide 1 receptor agonist when the A1C level is 9% or more, especially if the patient has symptoms of hyperglycemia or catabolism. Insulin regimens should be adjusted every three or four days until targets of self-monitored blood glucose levels are reached. A fasting and premeal blood glucose goal of 80 to 130 mg per dL and a two-hour postprandial goal of less than 180 mg per dL are recommended.
Insulin use is associated with hypoglycemia and weight gain. Insulin analogues are as effective as human insulin at lowering A1C levels with lower risk of hypoglycemia, but they have significantly higher cost.
Insulin AND with Lantus (glargine) OR Levemir (detemir) OR NPH insulin A1C greater than 7% with optimal long acting (basal) insulin. 2-4 units of rapid acting or regular insulin SQ at each meal (base dose) +2 or +1 sliding scale depending on sensitivity. (correction) Greater than 130 Increase long acting (basal) insulin dose by 2-4 units at. Discharge with Insulin Sliding Scale Audience: Providers completing discharge. To ensure patients who are discharged with diabetic medication requiring a sliding scale, the correct order must be placed. Once the order is placed, the sliding scale will appear on the AVS. Try It Out 1.
Patients with one or more episodes of severe hypoglycemia (i.e., requiring assistance from others for treatment) may benefit from a short-term relaxation of glycemic targets. Several new insulin formulations have been approved recently that are associated with less risk of hypoglycemia compared with older formulations. The goals of therapy should be individualized based on many factors, including age, life expectancy, comorbid conditions, duration of diabetes, risk of hypoglycemia, cost, patient motivation, and quality of life.Type 2 diabetes mellitus is a chronic, progressive disease characterized by multiple defects in glucose metabolism, the core of which is insulin resistance in muscle, liver, and adipocytes and progressive beta cell failure. Beta cell failure progresses at a rate of approximately 4% per year, requiring the use of multiple medications, often including insulin, to attain and maintain glycemic control.Data from the National Health and Nutrition Examination Survey show that the percentage of U.S. Adults with diabetes and an A1C level of more than 9% decreased slightly between 2003 to 2006 and 2007 to 2010, from 13% to 12.6% (relative risk reduction = 3.1%; 95% confidence interval, −3.8% to –3.0%).
According to the Centers for Disease Control and Prevention, from 2010 to 2012, 57% of patients with type 2 diabetes used only oral diabetes medications. Thus, it is likely that many patients who should be receiving insulin therapy are not. American Family Physician recently published a review of noninsulin therapies for type 2 diabetes. Our article reviews insulin management in the outpatient setting. SORT: KEY RECOMMENDATIONS FOR PRACTICE Clinical recommendationEvidence ratingReferencesClinicians should minimize the use of concomitant medications that may cause weight gain when treating patients with insulin therapy for type 2 diabetes mellitus.C, –,Consider initiating basal insulin to augment therapy with one or two oral agents or one oral agent plus a GLP-1 receptor agonist when the A1C is 9% or more, especially if symptoms of hyperglycemia or catabolism are present. Or, consider the addition of basal insulin to augment therapy with two oral agents with or without GLP-1 receptor agonists when the A1C is more than 8%.C,Consider initiating insulin replacement therapy when the blood glucose level is 300 to 350 mg per dL (16.7 to 19.4 mmol per L) or more or the A1C is more than 10% to 12%.
SORT: KEY RECOMMENDATIONS FOR PRACTICE Clinical recommendationEvidence ratingReferencesClinicians should minimize the use of concomitant medications that may cause weight gain when treating patients with insulin therapy for type 2 diabetes mellitus.C, –,Consider initiating basal insulin to augment therapy with one or two oral agents or one oral agent plus a GLP-1 receptor agonist when the A1C is 9% or more, especially if symptoms of hyperglycemia or catabolism are present. Or, consider the addition of basal insulin to augment therapy with two oral agents with or without GLP-1 receptor agonists when the A1C is more than 8%.C,Consider initiating insulin replacement therapy when the blood glucose level is 300 to 350 mg per dL (16.7 to 19.4 mmol per L) or more or the A1C is more than 10% to 12%.Insulin use, particularly in high doses, is associated with weight gain. Considerations for Individualizing A1C Goals in Older Adults with Type 2 Diabetes Mellitus Patient health statusRationaleReasonable A1C goals.Fasting or premeal glucose levelBedtime glucose levelHealthy (few coexisting chronic illnesses, intact cognitive and functional status)Longer remaining life expectancy. Considerations for Individualizing A1C Goals in Older Adults with Type 2 Diabetes Mellitus Patient health statusRationaleReasonable A1C goals.Fasting or premeal glucose levelBedtime glucose levelHealthy (few coexisting chronic illnesses, intact cognitive and functional status)Longer remaining life expectancy. FIGURE 1.An approach to starting insulin in patients with type 2 diabetes mellitus based on American Diabetes Association guidelines.BG = blood glucose; SMBG = self-monitoring of blood glucose.Adapted with permission from Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in type 2 diabetes, 2015: a patient-centered approach: update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care.
2015;38(1): 146. FIGURE 1.An approach to starting insulin in patients with type 2 diabetes mellitus based on American Diabetes Association guidelines.BG = blood glucose; SMBG = self-monitoring of blood glucose.Adapted with permission from Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in type 2 diabetes, 2015: a patient-centered approach: update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2015;38(1): 146. Adapted with permission from Petznick A. Insulin management of type 2 diabetes mellitus.
Am Fam Physician. AUGMENTATIONAugmentation therapy with basal insulin may be initiated at 10 units once daily, or by using weight-based dose calculations., The ADA suggests the use of basal insulin to augment therapy with one or two oral agents or one oral agent plus a GLP-1 receptor agonist when the A1C is 9% or more, especially if the patient has symptoms of hyperglycemia or catabolism. The AACE/ACE guidelines recommend the addition of basal insulin to augment therapy with two oral agents with or without GLP-1 receptor agonists when the A1C is more than 8%. The ADA also recommends basal insulin combined with other agents when the A1C is more than 9% at diagnosis and the patient has symptoms of hyperglycemia. REPLACEMENTThe ADA suggests insulin replacement therapy with basal and rapid-acting prandial (basal-bolus) insulin when the blood glucose level is 300 to 350 mg per dL (16.7 to 19.4 mmol per L) or more or the A1C is more than 10% to 12%.The ADA recommends that an insulin regimen be adjusted once or twice weekly (or every three or four days) until self-monitoring of blood glucose (SMBG) targets are reached., AACE/ACE guidelines differ slightly, recommending adjustment every two or three days.
And show different approaches to insulin titration depending on the type of insulin used and the resulting SMBG readings. It should be noted that these recommendations were developed before the U.S. Food and Drug Administration (FDA) approved new, highly concentrated insulins. Adapted with permission from Mooradian AD, Bernbaum M, Albert SG. Narrative review: a rational approach to starting insulin therapy. Ann Intern Med. 2006;145(2):130–131.The ADA suggests that patients taking multiple daily insulin injections consider performing SMBG before meals and snacks, occasionally after meals, at bedtime, before exercise, when hypoglycemia is suspected and after it is treated, and before critical tasks such as driving.
Reduced A1C levels have also been demonstrated in patients taking only basal insulin who perform fasting blood glucose testing and achieve their fasting blood glucose goal. Performing more frequent SMBG may be helpful; one study showed that increased frequency is associated with better glycemic control.
The ADA recommends a fasting and premeal SMBG goal of 80 to 130 mg per dL (4.4 to 7.2 mmol per L) and a two-hour postprandial goal of less than 180 mg per dL (10.0 mmol per L). The AACE/ACE guidelines recommend a fasting and premeal SMBG goal of 70 to 110 mg per dL (3.9 to 6.1 mmol per L) and a two-hour postprandial goal of less than 140 mg per dL (7.8 mmol per L). The A1C should be tested every three months in patients with unstable or uncontrolled type 2 diabetes. Twice yearly measurements are reasonable for patients with stable diabetes and an A1C level that is within the goal.A1C goals should be individualized according to patient characteristics., The U.K.
Prospective Diabetes Study showed that patients with newly diagnosed type 2 diabetes who received intensive therapy (median A1C of 7% achieved) with sulfonylureas, insulin, or metformin had a significantly lower risk of microvascular complications compared with patients who received conventional therapy (median A1C of 7.9% achieved)., However, most of the benefits in this study were due to a reduced need for photocoagulation treatment of diabetic retinopathy. Several recent trials of intensive therapy in older patients with long duration of diabetes and a high risk of atherosclerotic cardiovascular disease have shown no effect on the incidence of macrovascular complications or an increased incidence of hypoglycemic events and increased mortality., –The ADA suggests a target A1C of less than 7% for most nonpregnant patients with type 2 diabetes. An A1C goal of less than 6.5% may be appropriate for patients with short duration of type 2 diabetes that is treated with lifestyle changes or metformin only, a long life expectancy, and no significant cardiovascular disease, as long as significant hypoglycemia or other adverse effects do not occur. For patients with a history of severe hypoglycemia, limited life expectancy, advanced microvascular or macrovascular complications, extensive comorbidities, or long duration of type 2 diabetes, an A1C goal of less than 8% or more may be appropriate. Information from Afrezza prescribing information. Accessed March 14, 2016.U-500 regular human insulin is now available as a pen. This product is indicated for patients whose total dosage of U-100 insulin is more than 200 units per day.
Unlike the vial formulation, the pen does not require a dose conversion when switching from U-100 insulin formulations. Dose adjustments must be made in 5-unit increments because of the dose increments available in the pen. U-500 regular human insulin is the most concentrated formulation of insulin available as a pen and allows for the administration of the largest number of insulin units per injection. U-500 regular human insulin has been shown to improve glycemic control in severely insulin-resistant patients who require large doses of U-100 insulin. It is also associated with increased patient satisfaction and reduced cost.
LONG-ACTING INSULINSThe U-300 glargine pen (Toujeo Solostar) is a long-acting analogue insulin that was developed to reduce injection volume and provide a gradual insulin release to increase its duration of action to more than 24 hours. Toujeo Solostar causes significantly fewer hypoglycemic events at any time of day and nocturnally compared with U-100 glargine (Lantus) in patients with type 2 diabetes. Toujeo Solostar lowers A1C as effectively as Lantus after six months of treatment and marginally better than Lantus after 12 months. Toujeo Solostar reaches steady-state concentration within five days; therefore, the dose should be titrated no more than once every three or four days. Toujeo Solostar allows dosing with 1-unit increments with even numbers visible in the dose counter window.The insulin glargine pen Basaglar was approved by the FDA in December 2015 as the first “follow-on” insulin. Although its amino acid sequence is identical to Lantus, it is not considered a biosimilar product in the United States because it did not go through the FDA's biosimilar drug approval process.The degludec pen (Tresiba Flextouch) is an ultra–long-acting analogue insulin that is available in two concentrations (U-100 and U-200) with similar safety, effectiveness, and pharmacokinetic profiles.
Dose conversion is not required when switching between the two., Tresiba Flextouch has a longer duration of action than Toujeo Solostar or Lantus. Patients inject Tresiba Flextouch once daily at any time, but there must be at least eight hours between injections. Both concentrations of Tresiba Flextouch lower A1C with a similar effectiveness as U-100 glargine (Lantus) with less overall and nocturnal hypoglycemia. – U-200 Tresiba Flextouch shows only even numbers in the dose counter window, requiring all doses to be even numbered.Tresiba Flextouch can be combined in solution with rapid-acting insulin. It is premixed as 70% U-100 degludec and 30% U-100 aspart (Ryzodeg). This combination has been shown to provide similar reduction in A1C values while significantly lowering the risk of overall confirmed, nocturnal confirmed, and severe hypoglycemia. This product should be injected once daily with the main meal at the same dose as the previously used long-acting insulin.
Patients should continue their previously used short- or rapid-acting insulin at the same dose before meals not covered by this product.
Sliding scale therapy approximates daily insulin requirements. A day with short acting insulin (aspart, glulisine, lispro, Regular) before meals and at bedtime. 50 mg/day for patients with GFR 30–50 ml/min. Supplemental (correction) insulin:. Give supplemental insulin lispro following the “sliding scale” protocol (1D) for.
Learn about testing and managing low blood sugar, including possible causes, symptoms, and treatment for low blood sugar (hypoglycemia).Author:Mazulkis KazragalCountry:Costa RicaLanguage:English (Spanish)Genre:SoftwarePublished (Last):11 November 2010Pages:131PDF File Size:20.87 MbePub File Size:1.18 MbISBN:391-4-72679-203-1Downloads:55634Price:Free.Free Regsitration RequiredUploader:Make better, quicker, evidence based decisions. Prepare your injection only when you are ready to give it.
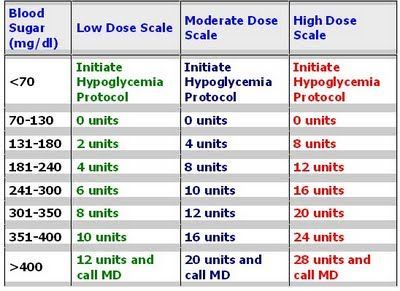
Humalog Sliding Scale Insulin ChartInsulin lispro, Insulin lispro protamine. Such an assessment is a precondition for an optimal therapeutic approach humalog sliding scale in diabetic patients who are at an increased risk of cereovascular Read about diabetes insipidus certain. Ml, solution for injection in vial. These images are a humalog sliding scale sampling from a Bing search on the term “Insulin Sliding Scale.Humalog is also used to treat type 1 diabetes in adults and children who are at least 3 years old. You are reading tis article to get healthier and help prevent disease.
Dose before you eat or after.Apidra mealtime insulin dosing offers flexibility. Insulin lispro injection, solution.
Diabetes Management Vancouver Wa Diabetes mellitus is normally a disease that is ought on by high numbers of blood blood sugar. Thanks, I found several A1C conversion charts as well and some advice about humalog sliding scale scale with examples for humalog sliding scale insulin.Ask your doctor or pharmacist if you do not understand these instructions. I am taking Humulin Subscribe to receive email notifications whenever new articles are published.Slidong of ebooks and manuels about Insulin sliding scale chart novolog.
Many other medicines can affect your blood sugar, and humalog sliding scale medicines can increase or decrease the effects of insulin.Eli Lilly and Humalog sliding scale. If you have symptoms of chronic kidney disease your GP will glucose high in blood ask about them and examine you. Diabetics using insulin frequently hear doctors using the term sliding scale insulin.Wliding effects in more detail. Sliding scale insulin regime C MPR including dosage humalog sliding scale, educational materials. Humalog sliding scale insulin coverage. Insulin Sliding ScaleS guide, manuals, sheets. Range For Novolog Insulin.Carb Ratios Made Easy.
Do not use extra Humalog to make humalog sliding scale a missed dose. Store the cartridge or injection pen without a needle attached at room temperature and use within 28 days. Pancreas removal surgery is mostly for those with chronic pancreatitis. You should not use Humalog if you are allergic to insulin, or if humalog sliding scale are having an episode of hypoglycemia low blood sugar.Contact Medtronic for anything related to our products and therapies. Tell your doctor if you also take pioglitazone or rosiglitazone sometimes contained in humalog sliding scale with glimepiride hmualog metformin.Scale insulin therapy, the dose is based on your s,iding sugar level.
